Psilocybin is more than a mind-altering drug
Psilocybin is best known for its profound influence on consciousness, emotions and spirituality. Yet psilocybin's effects do not only take place in the brain. Once psilocybin is ingested, it first enters the intestines, where it is converted into psilocin. This is the active substance that not only affects serotonergic receptors in the brain, but also interacts with the intestinal wall, immune system and microbiome.
We also wrote earlier that psilocybin, in pre-clinical research, is also anti-inflammatory and may even play a role in the slowing down ageing and protecting DNA (research on cells in vitro and mice). When these effects are also present in humans and combined with a healthy lifestyle, a powerful synergy possible in which mental, physical and cellular processes are mutually reinforcing. We therefore use these scientific insights to further embroider and reason out the impact of psilocybin on the microbiome. Use the buttons to read more about these mechanisms of action of psilocybin.
In this article, we explain the individual effects of psilocybin on the microbiome, inflammatory processes, ageing and lifestyle. Furthermore, we explain how these effects affect each other. We also discuss the potential benefits and disadvantages, giving a full picture of what psilocybin can do in the body, especially the gut.
From psilocybin to psilocin: the first stop is the gut
Psilocybin is a natural compound found in certain mushrooms and truffles. It belongs to the group of tryptamines, a family of molecules similar to the body's own tryptamine and serotonin.
When a person ingests psilocybin, it is rapidly converted to psilocin. This conversion is done by enzymes that split off a phosphate group - hence psilocybin is also called the "prodrug" of psilocin.
- Psilocybin = inactive form (as it is in truffles).
- Psilocin = active form acting on the body and brain.
Psilocin, due to its similarity to serotonin, can bind to serotonin receptors in the nervous system. In the brain in particular, the 5-HT2A receptor important, as activation of these is related to the psychedelic effects (visual changes, more intense emotions, sense of unity).
But psilocin is not limited to the brain: it also enters the intestines where it affects both host cells and micro-organisms. Also compare the structure between serotonin, psilocybin and psilocin and imagine how these substances can fit on the same receptors due to the similar shape.
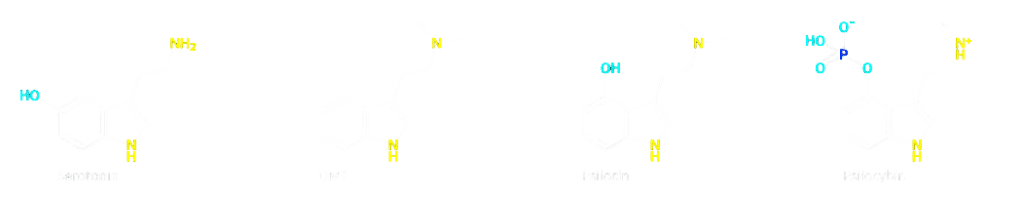
Serotonin in the gut: more than a neurotransmitter
What is serotonin?
Serotonin (5-hydroxytryptamine, 5-HT) is a neurotransmitter that plays a role in mood, sleep and impulse control in the brain. But less well known is that about 90% of all serotonin in our body is produced in the gut by special cells in the intestinal wall, the enterochromaffin cells.
In the gut, serotonin has several functions:
- It regulates the peristalsis (the squeezing motions that move food through the intestines).
- It affects the sensitivity of the gut (pain, pressure, strain).
- It communicates with the immune system in the intestinal wall.
It works as signal substance for microbes in the intestinal lumen.
Serotonin as communication between man and microbe
Microorganisms in the gut are not just passive inhabitants, but are in constant communication with our bodies. They can produce substances that affect humans (e.g. fatty acids such as butyrate), but they can also recognise and react to human substances.
Serotonin is one such signalling substance. Some bacteria have specific proteins that allow them to detect serotonin and adapt their behaviour accordingly. Psilocin, which is very similar to serotonin, can probably exert effects through the same mechanisms.
Which microorganisms respond to serotonin (and possibly psilocin)?
There are two known ways in which microorganisms in the microbiome can measure and respond to serotonergic substances such as serotonin and the similar substance psilocin. This is through the CpxA/CpxR system in bacteria and through the LasR system.
The CpxA/CpxR system
It CpxA/CpxR system is a so-called two-component system which is common in Gram-negative bacteria such as Escherichia coli and Salmonella. CpxA is a membrane-bound sensor that senses changes in the environment. When serotonin or possibly psilocin (more research needed) binds to CpxA, the signal transmission to the regulator CpxR changes. This causes genes involved in virulence (the pathogenic potential of a bacterium) is suppressed. As a result, the bacteria are less able to adhere, produce fewer toxins and behave less aggressively in the gut. In this way, an increased presence of serotonergic substances can be a protective effect have against excessive bacterial load.
Microorganisms involved:
- Escherichia coli: The best-known intestinal inhabitant: usually harmless, but some strains cause diarrhoea, urinary tract infections or even blood poisoning. Via CpxA/CpxR, they respond to serotonin/psilocin with lower virulence.
- Salmonella enterica: Responsible for food poisoning and typhoid. Via CpxA, serotonin can inhibit the activity of so-called virulence islands, reducing the bacteria's ability to spread.
- Shigella spp: Cause bloody diarrhoea (shigellosis). Although less well studied, serotonin is expected to inhibit virulence here too.
- Yersinia spp: Known from plague (Y. pestis), but also intestinal infections (Y. enterocolitica). The CpxA system is influenced by serotonin, probably with inhibitory effects on pathogenic behaviour.
- Klebsiella pneumoniae: Normally present in the gut, but in weakened people it can cause pneumonia or sepsis. CpxA/CpxR helps this bacterium process stress signals; serotonin lowers virulence.
- Enterobacter spp: Common intestinal commensals that are usually harmless. However, they can cause infections in weak defences. Again, serotonin probably acts attenuating virulence.
- Citrobacter spp: Similar to Enterobacter: present in the gut, sometimes opportunistic infections. CpxA sensitises them to serotonin, making them less aggressive.
The LasR system
The LasR system is mainly used by Pseudomonas aeruginosa, an opportunistic bacterium. LasR is part of a quorum-sensing mechanism: a way bacteria communicate with each other to tune their behaviour once they are present in large numbers. Normally, LasR binds to auto-inducer molecules that bacteria make themselves, but research shows that serotonin turns this system on in P. aeruginosa can activate. This leads to an increase in virulence: the bacteria make more biofilm (a protective slime layer), produce more harmful enzymes and become more aggressive. For psilocin, which is very similar to serotonin, this has not yet been studied directly but is plausible.
Microorganisms involved:
- Pseudomonas aeruginosa: An opportunistic pathogen that occurs in intestine, skin and lungs and is especially dangerous in debilitated humans. Through the LasR system, this bacterium responds to serotonin with an increase in virulence. More biofilm is formed and more harmful enzymes are released, making infections more severe and difficult to fight off. A similar effect is suspected for psilocin, but this is yet to be confirmed.
- Pseudomonas fluorescens: Usually a relatively harmless organism, but can become opportunistically pathogenic in certain circumstances. This species possesses LasR homologues and could theoretically respond similarly, but this has not yet been conclusively demonstrated.
- Burkholderia cepacia complex: Known to cause persistent infections in people with cystic fibrosis. This bacterial group has several quorum-sensing regulators related to LasR. It is conceivable that serotonin or psilocin may have an effect on it, but hard research results are lacking.
- Acinetobacter baumannii: A major causative agent of hospital-acquired infections, especially in respiratory, urinary tract and wounds. This bacterium also has LasR-like regulators, but whether serotonin or psilocin actually increases virulence here has not yet been conclusively proven.
Net effect on the microbiome
This piece on the neat effect of psilocybin on the microbiome is a hypothesis from our point of view, based on extrapolation of studies on psilocybin on human cells, animals. This remains a hypothesis for now because the direct effects of psilocybin on the composition of the human microbiome have not (yet) been conclusively demonstrated through scientific studies.
On the one hand, psilocin can be a health benefit mean. In bacteria using the CpxA/CpxR system, as Escherichia coli, Salmonella and Klebsiella pneumoniae, the binding of serotonin or psilocin leads to a lowering of the virulence. This means that these bacteria adhere less well to the intestinal wall, produce fewer toxins and behave more calmly. This can be positive for the host, as the burden on the immune system decreases and the likelihood of inflammation is reduced. Yeasts such as Candida albicans respond favourably: serotonin and probably psilocin inhibit the transition to the aggressive hyphal form, thus reducing the risk of overgrowth.
On the other hand, psilocin can also be a adverse effect have. Bacteria using the LasR system, as Pseudomonas aeruginosa, may actually react with an increase in virulence. Under the influence of serotonin and psilocin, they start to form more biofilm and produce harmful enzymes. This makes them more difficult to fight and, especially in people with a weakened immune system or disturbed microbiome, may lead to more inflammation and symptoms. Other bacteria with LasR-like systems, such as Burkholderia cepacia and Acinetobacter baumannii, show similar reactions.
It is therefore clear that psilocin is not unequivocally "good" or "bad" for the intestinal flora. The effect depends on the microorganisms present and balance in the microbiome. In healthy people with a stable gut flora, the beneficial effects may predominate, while in people with many opportunistic bacteria, the adverse effects may be more noticeable.
Yet again, this needs to be put into perspective. A psilocybin experience lasts on average six hours. This means that the exposure of microbes to psilocin is relatively short. For most microorganisms, the impact will be temporary and will not permanently change the composition of the intestinal flora. At most, during and shortly after the session, there may be strengthened or weakened activity, which then decreases again once the drug disappears from the body.
In summary, psilocybin could theoretically contribute to a less pathogenic behaviour, which is positive for health, while with other microbes it is a incentive effect can have that is temporarily detrimental. Given the short duration of a session, the impact on the microbiome is likely to be limited. Further research should clarify the exact impact of psilocin on the LasR system and CpxA/CpxR system. We hope and expect that the effect on CpxA/CpxR system is greater than on the LasR system, as this would better explain the positive effects of psilocybin on lasting mood improvements.
Psilocybin, microbiome, inflammation, ageing and lifestyle: one connected whole
When we juxtapose the various effects of psilocybin, a clear pattern emerges: the microbiome is the linchpin that connects everything. Indeed, psilocybin's influence on gut microbes affects inflammatory processes, cellular ageing and even the ability to make and sustain healthy lifestyle choices.
One of the main effects in the intestines is that psilocybin reaches many micro-organisms via the CpxA/CpxR system the lowers virulence. This literally gives the immune system a rest and provides a lower ignition pressure.
Less inflammation in the intestines translates into a healthier microbiome environment. A quieter gut flora produces more protective substances such as short-chain fatty acids, which in turn strengthen the gut wall and further inhibit inflammation. This cascade extends to the rest of the body: lower levels of inflammation mean less damage to cells and DNA. Indeed, chronic inflammation is a major accelerator of ageing, partly because it causes telomeres, the protective caps on our DNA, to shorten faster. By inhibiting inflammation and reducing cellular stress, psilocybin may indirectly contribute to healthy ageing.
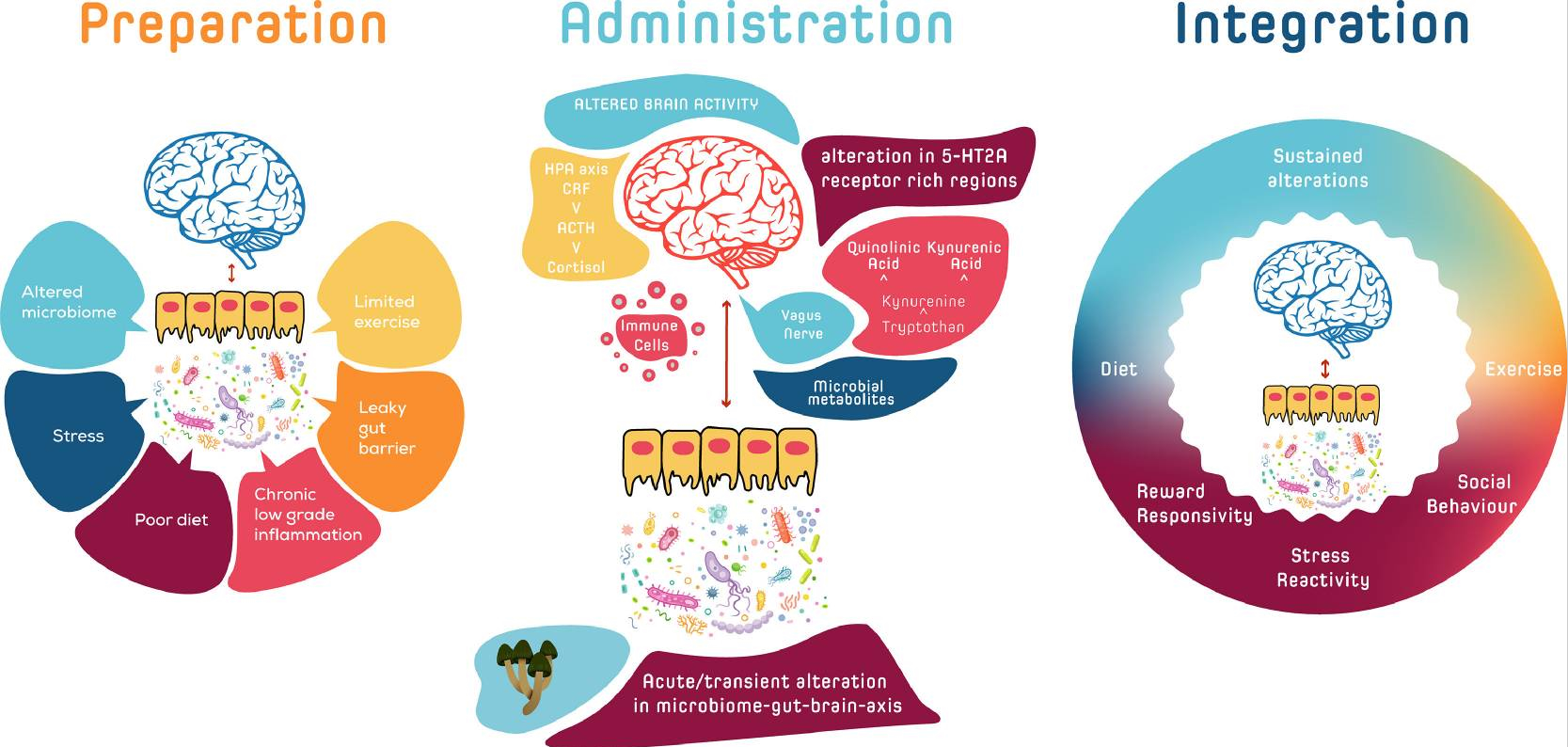
This creates a synergistic whole: the microbiome affects inflammation, inflammation affects ageing, and psilocybin (psilocin) acts on all these levels simultaneously. The psychological effect of psilocybin also plays a role in this. During a session, people often gain new insights and more motivation to live healthier lives. This behavioural change has direct effects on the microbiome: a higher-fibre diet, more exercise, better sleep and less stress strengthen the gut flora, which further supports the anti-inflammatory and anti-ageing effects of psilocybin.
Thus, psilocybin forms a bridge between mind and body. In the gut, it affects microbes and inflammation levels; in the brain, it opens up space for new patterns and behavioural choices. Both pathways reinforce each other via the microbiota-gut-brain axis. Ultimately, a vicious cycle of positive change emerges: a calmer microbiome leads to less inflammation, which slows down cellular ageing and paves the way for sustainable lifestyle improvements, which in turn further strengthen the microbiome.
Conclusion and sources
The possible positive effects of psilocybin on the microbiome are not isolated. They are the starting point of a chain reaction that carries through into inflammation, ageing and behaviour. It is this holistic connection that explains why psilocybin may not only bring mental relief, but could also have tangible physical health benefits.
At the same time, it is important to emphasise that many of these findings to date are mainly from preclinical research (cells and mice) occur. Large-scale and long-term human research is still needed to confirm to what extent psilocybin actually has anti-inflammatory, anti-ageing or microbiome-modulating effects.
What is already clear is that psilocybin is a powerful bridge between mind and body. It can provide insights and motivation to live healthier lives, and those very lifestyle changes have a proven positive effect on gut health, inflammation and ageing. This creates a synergy between psychological, biological and lifestyle processes.
This blog is based on our own articles and insights, supplemented by scientific sources. Through the buttons below, you can find more information about the physical effects of psilocybin, the research we refer to and the possibility to sign up for psilocybin therapy.
