Stopping a bad trip
Stopping a bad trip with medication is sometimes possible, but medication is not the first step that needs to be taken immediately. In the case of a difficult or frightening psychedelic experience, it often works better to first ensure calm, safety, and proper guidance. A calm guide, a safe environment, fewer stimuli, reassurance, a different body posture, appropriate music, and a supportive presence can already make a big difference. Sometimes it also helps to provide more physical stability, for example with some dextrose and GABA. Taking these substances can often provide just that little bit of calm so that the bad trip turns into more peace. Therefore, not every difficult trip needs to be stopped immediately with medication.
That is also logical, because a challenging start to a trip does not necessarily have to end badly. Especially at the beginning, tension, anxiety, or confusion can sometimes be part of a process in which old tension is triggered. If a sense of breakthrough, relief, or victory follows, such a difficult start can even prove to be very valuable. A difficult phase, therefore, does not automatically mean that the session is a failure or is dangerous. The difference often lies in the level of guidance, manageability, and whether someone remains approachable and safe.
Why a trip can be challenging, especially the beginning
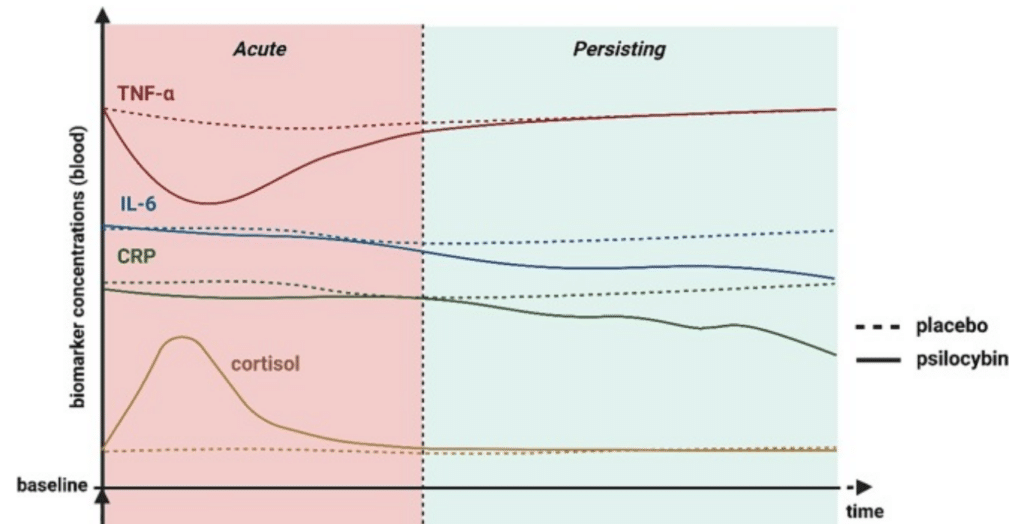
A trip can feel challenging because a lot changes simultaneously in body and mind in a short period of time. Biologically speaking, with various psychedelics, including psilocybin, you often first see an increase in cortisol, as is also visible in the image. Cortisol is a stress hormone and can temporarily cause restlessness, tension, or a sense of alertness, but this usually subsides as the experience unfolds. At the same time, glutamate is also affected, an important signaling molecule involved in stimulus processing, learning, and brain activity, which can cause thoughts to become more intense, associative, or less predictable. This means that the beginning of a trip can sometimes feel physically restless or mentally overwhelming, even without anything being immediately wrong.
In addition, emotions that normally remain in the background may surface, whereas people naturally often resist truly allowing sadness, fear, shame, or old tension. The grip on time, self-esteem, and reality can also diminish, partly because the activity of the default mode network (DMN) decreases. This network normally helps maintain a stable narrative about oneself and the world. When that temporarily loosens, it can be liberating, but initially also confusing or unsettling. Added to this is the fact that the experience is often new, and people naturally resist the unknown as well. A challenging trip is therefore often a temporary combination of biological activation, emotional release, reduced control, and entering unknown inner territory.
These disruptive effects occur primarily during the emerging phase of the trip. If people show too much resistance or cling too tightly to the familiar, this can lead to a challenging start. If the resistance persists throughout the entire trip, it is called a bad trip.
When medication comes into play
Medication only truly comes into play when non-pharmacological support is insufficient or when the situation threatens to become unsafe. Examples include severe panic, disorientation, dangerous behavior, persistent agitation, or the complete loss of contact with the psychedelic facilitator. In such cases, the goal is no longer to help someone through the difficult phase, but to reduce the intensity or truly terminate the psychedelic state.
Furthermore, there is an important distinction between substances that primarily calm a person and substances that substantially weaken the psychedelic effect itself. This distinction is often insufficiently made in the literature. Making someone calmer is not the same as actually stopping the trip.
The best real trip stopper is ketanserine
If the goal is truly to pharmacologically stop a classic serotonergic trip, such as that caused by LSD, psilocybin, DMT, or mescaline, then ketanserine emerges as the strongest candidate. The reason is that ketanserine blocks the 5-HT2A receptor, which is precisely the key receptor through which classic psychedelics produce their characteristic effects. As a result, ketanserine is not only a sedative but also a substance that can inhibit the core of the trip.
According to This research shows that ketanserine is the best, real trip stopper.. The main disadvantage is that it is not readily available everywhere and that it can lower blood pressure. Nevertheless, from a pharmacological perspective, this is the most direct choice if one wishes to purposefully end a classic psychedelic state.
Risperidone is the best practical alternative
Because ketanserin is not always available in practice, risperidone is often considered the best practical alternative. Risperidone is better known and more readily available in the Netherlands, and is trusted by physicians as a medication for acute psychiatric situations. Risperidone also has a strong effect on the 5-HT2A receptor and can therefore do more than just sedate.
If ketanserine is unavailable, risperidone is likely the most logical pharmacological option to mitigate the substance of a bad trip. That does not necessarily make risperidone pharmacologically better than ketanserine, but it does often make it more realistic to use.
Not every trip stopper really stops the trip.
There are also other substances that are sometimes used, such as olanzapine, quetiapine, trazodone, mirtazapine, or benzodiazepines like diazepam and lorazepam. These can be useful in certain situations, but they do not all have the same function. Benzodiazepines primarily reduce anxiety and tension and can make a person calmer, but they usually do not actually stop the psychedelic experience. Quetiapine is also often mentioned by users, but this seems to be partly because it has a sedating effect. However, sedation is not the same as a receptor-targeted trip stopper.
Someone can become sleepier and calmer due to various medications, but still be in a psychedelic state. If the goal is truly to end the trip itself, then ketanserine and risperidone are much more logical agents than just a sedative.
Why the circumstances must be adjusted first
In practice, many bad trips are caused not only by the substance itself, but also by the combination of tension, anticipation, the environment, and a lack of support. That is precisely why adjusting the setting can often make a surprisingly big difference. Different music, less light, fewer people in the room, a familiar voice, more physical rest, and reducing cognitive overload can often already bring someone back to a greater sense of safety. Sometimes it also helps to support the body with a little sugar + GABA or a calming protocol, as long as this is done carefully and fits within the guidance provided.
In guided sessions, this is often the first and best option. Many people who seem to be panicking eventually break through the difficult layer when they feel safe again. What initially appeared to be a breakdown turns out, in retrospect, to have been an intense but meaningful part of the session.
A difficult trip is not always a bad trip
That is perhaps the most important nuance. A trip can start out confronting, chaotic, or emotionally heavy, yet still result in something healing. Especially when someone moves through fear and subsequently experiences relief, insight, or a sense of victory, the session can actually yield significant results. You see this more often when the guidance is good and the person is not taken out of the process too quickly.
Medication should therefore not be used out of haste or to inconvenience those around it. It should be a means for situations where safety or stability is truly at risk, not for every difficult emotion or every challenging phase. Sometimes the art lies precisely in helping someone continue to function well, rather than stopping immediately.
Also pay attention to preparation and neurochemistry
You cannot prevent a bad trip solely with the right dose or a good guide, but above all with good preparation. Many difficult experiences do not arise purely from the substance itself, but from the combination of tension, uncertainty, physical restlessness, hidden emotions, and an environment that does not align well with what someone needs. Preparation helps to minimize these risk factors even before the session. If someone knows what can happen biologically and psychologically, restlessness, emotional fluctuations, or a distortion of time and self-perception are less likely to be perceived as a danger. That alone can prevent a lot of panic.
At Triptherapie, we also pay close attention to neurochemistry during the preparation. Research has shown that relatively too much glutamate and too little GABA can be an important factor in negative experiences. Glutamate is associated with irritability, mental activation, and sometimes a feeling of being agitated or overstimulated, whereas GABA supports more calm, inhibition, and stability. If someone starts a session already tense, poorly rested, or neurochemically unbalanced, a psychedelic experience can be perceived more quickly as too intense or threatening. That is precisely why we pay attention to factors such as sleep, stress levels, nutrition, supplements, medication, stimulants, and the overall resilience of the nervous system.
Good preparation also means looking at intentions, mental resilience, physical condition, medication use, sleep, and nutrition beforehand. Additionally, it helps to discuss in advance how you handle fear, loss of control, or emerging emotions. Those who learn beforehand that resistance often creates more tension and that surrender can actually bring space have more stability during the trip. Preparation, therefore, does not ensure that a session will always be easy, but it does ensure that difficult moments are less likely to turn into a real bad trip.
Conclusion
Stopping a bad trip with medication may sometimes be necessary, but proper guidance always remains the most important first step. Rest, safety, appropriate music, reassurance, reduced stimuli, and physical regulation can already make a big difference, and sometimes even a difficult start can turn into a valuable experience if relief, insight, or a sense of triumph follows. Not every challenging trip is therefore a failed trip, and that is precisely why medication should not be used too quickly.
If pharmacological intervention is nevertheless necessary, the literature discussed primarily indicates that ketanserine is the best true trip stopper, with risperidone as the best practical alternative when ketanserine is unavailable. These agents make more sense than relying solely on sedatives, as they act more strongly on the mechanism of action of classic psychedelics. At the same time, this topic also demonstrates the importance of preparation. Therefore, at Triptherapie, we look not only at the dose and setting, but also at factors such as stress, sleep, medication, emotional strain, and neurochemical balance, where a state of relatively too much glutamate and too little GABA can increase the likelihood of a negative experience. The best protection against a bad trip, therefore, does not begin with a trip stopper, but with careful preparation, proper guidance, and only then—if truly necessary—the right medication.
Disclaimer
The information in this article regarding stopping a psychedelic experience with substances such as ketanserine or risperidone is based on theoretical and pharmacological insights. Please take the following into account:
Only via a doctor: These medicines fall under the Medicines Act and may only be prescribed and administered by a qualified doctor. Combining psychedelics with this strong medication independently can be dangerous.
Current practice vs. theory: Although ketanserine and risperidone are theoretically the most effective 'trip stoppers' because they act directly on serotonin receptors, they are rarely used for this specific purpose in current medical practice.
Current emergency procedures: In acute emergency situations (such as extreme panic or a bad trip in the emergency room), benzodiazepines (such as diazepam or lorazepam) are currently still chosen more frequently. These medications do not stop the substance of the trip, but have a calming and anxiety-reducing effect to make the situation manageable.
Future outlook: As psychedelic therapy becomes more standardized and takes place more frequently in medical settings, it is possible that specific receptor blockers such as ketanserin will play a larger role in the future.
Therefore: In the event of a difficult experience, always rely first on good guidance, a safe environment, and techniques that help with relaxation. For medical concerns, always seek professional help and never experiment with prescription medication on your own.